Help for Those Who May Run or Wander Off
By Cristen Carson Reat
If I Need Help Offers Creative Low Tech Solution for Those Who May Run or Wander Off

So it happened one day when we weren’t expecting it. We weren’t expecting it because my son Vincent is not a wanderer or a runner. One spring afternoon when the whole family was home, an open door was discovered, and my 11-year-old son with an intellectual disability was GONE.
A stranger knocked on our door asking if we were the parents of a little boy in a wheelchair with blue glasses? Though Vincent does not use a wheelchair on a regular basis, we use an adaptive stroller when we take frequent family walks. A kindly neighbor whom we did not know discovered my son walking bare feet in our neighborhood and knew something was not right. Though he is verbal, he refused to give an unknown adult his name and address, instead chose to sit in the middle of the street uncommunicative. Thankfully, he was unhurt, though confused with all of the fuss – and we will forever be grateful to a kind-hearted neighbor.
Until that moment, I did not have the constant worry that Vincent may run or wander off, but many families struggle with the daily challenge of managing children or adults who are wanderers. Those with cognitive impairments or limited verbal skills complicate this already frightening scenario.
The Problem
Living in a large urban area, I have seen as many Silver alerts as Amber alerts on billboards across the city, indicating missing seniors or children. Many families I know struggle with the stress of managing an individual who may run or wander off, and in recent years there have been improvements in devices to help track individuals who go missing.
However, when I began to research possible technology solutions following our incident, I found several paid finder/location services available for those who wander – including pet tracking – which require the wearing of a bracelet, tag or some kind of GPS device. The expense of monthly monitoring, that works much like a home security service, was more than we wanted to pay or needed. I doubted that my son who has many sensory issues would agree to wear a bracelet or cumbersome tracker on his clothing, so I was more interested in a low-tech solution that made sense for our situation. That is when I discovered If I Need Help.
The Brilliant Low Tech Solution for those who may run or wander off
If I Need Help is a parent created non-profit organization that works by using QR Code technology. QR is short for Quick Response and can be read quickly by a smartphone. You may have seen QR codes in magazine advertisements, store receipts, a billboard, web page or even someone’s shirt. Once a QR code is scanned, it will show you a clickable URL (website address) to view additional information such as a trailer for a movie, a coupon for a store. Or, in this case, personalized information entered into a secure profile by parents or caregivers. The advantage for caregivers and law enforcement is that scanner apps are free and easily installed onto a smartphone.
If I Need Help creates personalized wearable QR codes in the form of patches, pins, clips, ID cards, shoe tags and more that can be scanned or entered into a secure website to view a live profile. It can be updated in real time and emailed to others, including law enforcement, if a search is needed.
Customizing If I Need Help for My Son – The Set Up
- Creating an Account. Signing up for a free account and setting up a profile took under three minutes.
- Completing a Detailed Profile. An optional Q&A form can be created, stored, modified at any time, and emailed to first responders, emergency personnel, searchers and other important people. Filling this form out took about 30 minutes, as it includes helpful details crucial in interacting with someone who is lost, scared and stressed. This information ranges from important medical information, communication information (such as verbal or non-verbal), necessary equipment, and helpful phrases to favorite books, characters or a reassuring song, and calming techniques to be used with that individual. I had gathered most of this information, including medical, already stored on an app, so it was at my fingertips and easy to copy and paste into the web-based form on the If I Need Help If you must gather this data from multiple sources, this will add to your set up time.
- Selecting the Product. There are a variety of products available to fit nearly every imaginable need from pins, ID cards, shoelace tags, key chains, patches, magnets, shirts, bumper stickers, hoodies, hats and more. Because Vincent struggles with sensory issues I assumed a patch would bother him, a pin unsafe, a bracelet would not be tolerated and because his shoes did not have laces, he could not wear the shoelace identifier. Finally we settled on stickers and a shirt.
Peace of Mind
Why not just use a medical alert bracelet to help those who may run or wander off? Many people have worn and used medical alert bracelets successfully, but companies sometimes charge an annual fee and some individuals simply cannot tolerate wearing a bracelet, such as those with autism, sensory issues, or certain medical conditions. If I Need Help offers a simple, yet powerful solution for as low as $2.00.
Does Vincent wear a patch every day? No, but for those times that our family travels, he goes on a field trip or we make a trip into crowded places in the community such as a museum, park or zoo, using these products give us peace of mind.
Bridging the gap between technology and people with disabilities.
BridgingApps, a program of Easter Seals Greater Houston, is a community of parents, veterans, therapists, doctors, educators, and people with disabilities who share information on how apps and mobile devices can help people of all abilities reach their highest levels of physical, social and cognitive development.
Special Needs Planning: 3 of 3
Part 3 – Failing to Take Action

For the past two days I have talked about why planning for the future of your loved one with a disability is so crucial, and the consequences of what happens when you don’t plan. The following poignant case studies illustrate my point. These are true stories of circumstances that could have been prevented by taking some simple planning steps. Don’t let yourself and your loved one become another story of the consequences of not planning.
Divorce
Marc and Amy divorced about 18-months after Kenny was born. The divorce was not pleasant, but it was not a war either. Marc agreed to Amy having custody of their two children. Kenny, who has Cornelia de Lange Syndrome, is the youngest.
Marc paid alimony and child support regularly for the first few months. His bi-monthly visit to the children became less and less frequent. Support checks arrived late, and sometimes not at all. Marc remarried about two-years later and moved to another state. The support checks stopped altogether as did the visits and holiday cards. Amy was “on her own.”
Amy’s family helped. Even Marc’s parent’s provided some financial assistance. Amy inherited $300,000 from her grandfather. This was a tremendous help, as it allowed her to work fewer hours at her job and spend more time with Kenny.
Kenny was 12-years-old when Amy was diagnosed with breast cancer. Surgery and months of chemotherapy and radiation were unsuccessful. Believing she would not die, Amy did not make any provisions for her estate or children.
After Amy’s death, Marc, being the biological father, was given custody of the children even with his history of defaulting on child support, and not having seen the children in years. He also received control of Amy’s estate. Could this have been his motivation to get custody of the children? Control of their inheritance? Is Marc truly the best person suited to care for these children? Do you think this is what Amy wanted?
What could Amy have done to avoid this situation? There was no guarantee that Marc could be kept from getting custody of the children. Amy would have been wise to keep a journal of missed support checks, the infrequent calls and visits, and how Marc voluntarily estranged himself from the children. At least other family members would have had a strong case to contest Marc’s appointment as guardian and trustee. However, Amy could have guaranteed that Marc would have no access to, or control of the money she left her children. A Special Needs Trust for Kenny and a traditional Trust for her other child, would have a Successor Trustee appointed by Amy, to manage and control the funds for the benefit of the children and out of the hands of Marc. The Successor Trustee also has sole discretion in disbursements from the Special Needs Trust.
Amy might have been able to convince Marc to rescind his parental rights leaving her able to appoint a Successor Guardian/Conservator of her own choice. Regardless, she should have discussed this with him. She could have stated what she wanted for Kenny and made the necessary arrangements while she was still able.
If Marc violated his duties as Trustees and misused the assets in the trusts he would have been liable for criminal charges. However, the likelihood of the money being replaced is zero to none. A big problem was ignored. The opportunity to resolve it easily was gone. This is a common occurrence.
Bubba, Bubba, Bubba
Michael is 42-years-old and lives with his mother, Anne. Michael has multiple disabilities. His communication and functioning skills are at the level of a two-year-old. He uses a wheelchair and requires assistance for all of his needs. Anne has cared for him his entire life.
Michael is able to speak a few words. One of the things he does is roll his head from side-to-side, smile and say, “Bubba, Bubba, Bubba.” I asked Anne what Michael meant. “What do you think it means?” she responded. I told her I had no idea. Anne said, “Bubba, Bubba, Bubba means “bubbles!” So I assumed Michael wanted Anne to blow bubbles for him. Anne further explained, “It’s bubbles in a soft drink. He likes the tickle in his throat when he drinks it.”
It is a cute story, however, it made me think. Anne had done no planning. There was no written information or instructions for Michael’s care needs. Imagine if Michael came to live with you and you have to figure everything out yourself. You watch him roll his head and hear Michael say, “Bubba, Bubba, Bubba” a few times each day. What would you think he meant? After a few days he says it again, this time without a smile and fewer times each day. By the end of two weeks he never says it again.
Michael’s limited communication skills allowed him to express a desire for one of the few things that made him happy and gave him pleasure. Who knows what self-esteem he felt because he was able to make a request and have it understood and fulfilled. What a tragedy it would be if Anne died and never let anyone know about, “Bubba, Bubba, Bubba.” Think about how well and secure Michael would feel, if after losing his Mother, being moved from his home, and changing his life completely, he says to his new care providers, “Bubba, Bubba, Bubba,” and they know to give him that favorite soft drink. How do you think it would make Anne feel if she could see Michael’s smile?
It is a touching story, however, it made me think, “What happens if like in Anne’s case, you had done no planning?” As in Michael’s situation, there was no written information or instructions for your loved one. Imagine if Michael came to live with you, and you had to figure everything out yourself. You watch him roll his head and hear him say, “Bubba, Bubba, Bubba” a few times each day. What would you think he meant? After a few days he says it again, this time without a smile and fewer times each day. By the end of two weeks, he never says it again. I addressed earlier the reality of mortality and the fact that your child may very well survive you. You will not be gone for “just a few hours.” You are gone permanently.
My intention these past three days has been to help you appreciate and understand how dire the consequences will be for your loved one with special needs if you have not done any future planning for them.
These two stories make abundantly clear that the person you are hurting by not doing special needs planning, is your loved one with special needs. Who better than you to know and understand their wants and needs? They are relying on you to take care of them, because they cannot take partial or full care of themselves.
Those attending my seminars or hearing my presentation at a conference, ask afterwards where they could get the most up-to-date information I presented? That’s why my partner Bart Stevens finally wrote, “The Beginner’s Guide to Special Needs Planning©, originally released in November 2002 and updated in January 2018. The book removes the obstacles in planning, answers your questions, and guides you through the planning process in a simple, step-by-step method. It takes an overwhelming process and breaks it down into simple steps that you can easily understand. After reading this book, you will be prepared to begin the actual planning process. Contact us for your copy.
Planning today will eliminate your concerns so you can be assured that your loved one with special needs will have the best care, security, and quality of life possible. Don’t delay, visit www.SerenitasSNP.com, or call 818-231-6759 today.
If I NeedHelp makes wearable iD and offers a free Caregiver controlled special needs registry for our loved ones who may wander or need assistance in a critical moment.
Special Needs Plan: Part 2 of 3
Part 2 – Did You Know?

Yesterday, I talked about why planning for the future of your loved one with a disability is so critically important. Today, I want to talk about what proper planning can actually accomplish. What it really means.
With proper planning, you will decide who will care for your child; where they will live; who will manage assets left for their care; the type of care he or she will receive; and what your specific wishes and goals are for your loved one. If you do not plan, these decisions will be made by the state in which your loved one lives and those who will be appointed to provide care and supervision. You have no assurances that what you want for your loved one will be done.
Stop for a minute and think about what would happen tomorrow if you were not here.
Review all the things you do each day for your loved one. Dressing; feeding; getting them off to school, work or the adult center; knowing their dietary needs; how to communicate; and all the other “little” details. This information must be given now to current providers (teachers, therapists, medical practitioners, case workers) and those who will serve in the future (guardians, trustees, conservators). Do you want the people who provide care and protection for your child to have to figure everything out on their own? What if they can’t figure it out? What effect will this have on your child? Is it fair to them or your child not to plan now before it’s too late? Creating the Letter of Intent, does just this. It’s not a legal document, merely the instrument to provide comprehensive information to current and future providers about your loved one’s abilities and requirements. This is a document that should be updated each year as your loved one grows and his or her needs change.
How can you provide for the supplemental needs of your loved one with a disability without jeopardizing their Social Security and healthcare benefits?
Why is it so important to make family and friends aware of the planning you have done for your loved one? How is it possible that one well meaning person can throw a “monkey wrench” into all the careful plans you have made and jeopardize your loved one’s Social Security and healthcare benefits, and result in the loss of assets left for his or her care? By creating a Special Needs Trust to hold, manage and protect the assets you leave for your loved one, you will ensure them a lifetime of care and supervision. By setting-up the correct Trust, family and friends can put their assets into the Trust while still living. Not all Trusts allow you to do that.
When you set-up a Special Needs Trust, your loved one with a disability is the beneficiary of the Trust. Why is this so important? Because some families are concerned that should a Special Needs Trust be established, and their loved one with a disability becomes self-sufficient and no longer needs the Trust funds, the money is no longer available to them. What happens? The money can be used for their college education, a home, a car, to start a business, anything they want to use it for.
In addition to the above, let’s look at what else you can accomplish with the proper planning. No planning, or improper planning can have dire consequences, including:
- All the guardians/conservators and trustees and their successors can be chosen ahead of time. You can even ask your child with special needs who they would like to take care of them after your death. What peace of mind for you knowing that your loved one will have guardians and trustees of your choosing taking care of them.
- Not all assets pass through a Will. Life insurance, retirement plans and annuities pass by beneficiary designation. Your child could receive these assets even if they are not named as a beneficiary. With proper planning, a serious potential problem can be averted.
- If the State is unable to find a single home for all of your children, they could be forced to live in separate homes.
- Your Estate will be distributed according to the rules of “Intestacy” in your State of residence. You have no say in this matter. If you are divorced from your child’s biological parent and remarried, your current spouse receives all your personal property and can do anything they want with it. If you are unmarried, your children share your Estate equally. Either way, your loved one with special needs may not get enough to live on, or anything at all.
- Regardless of how much in assets your loved one receives in their name, this money is subject to an immediate payback to Medicaid for previously provided healthcare services.
- In addition to the payback to Medicaid, if the person’s remaining assets exceed $2,000, they will be ineligible for Supplemental Security Income (SSI) and Medicaid. The result is the loss of part, or all of their inheritance, ineligibility for SSI cash benefits and healthcare through Medicaid.
- Your child’s standard of living could be seriously jeopardized with the loss of these benefits and assets. To make matters worse, there are no budgetary guidelines to know exactly what your child’s monthly income requirements will be.
Are you starting to get the picture as to why future planning for your loved one with a disability is no longer an option? You must take responsibility and begin the planning process today. What I’ve talked about is only the tip of the iceberg. If you don’t do proper planning, you can see the problems you are creating for your loved one with a disability. No one wants to think about his or her own mortality. It’s downright scary. But don’t you want to make your loved one’s transition after your death as easy as possible? Discover the solutions for today, tomorrow and the future, by visiting Serenitas Special Needs Planning at www.SerenitasSNP.com, or call 818-231-6759. Make the commitment today.
If I NeedHelp makes wearable iD and offers a free Caregiver controlled special needs registry for our loved ones who may wander or need assistance in a critical moment.
Special Needs Planning: Part 1 of 3
Part I – What If?

If you have a child with special needs or another relative in your care who has a disability, have you considered what will happen to your loved one if you make no plans for their future care when you die or are no longer able to provide the care and supervision he or she requires? It doesn’t matter if your loved one is three-months old or 70-years-old. Whether you are a couple or a single parent in your 20’s, 30’s, 50’s or 80’s, or if your annual income is $25,000 or $25,000,000. What matters, is the fact that Special Needs Planning is a responsibility that must be addressed now, before it is too late. Your plan should be based on the abilities and needs of your child today, not what you think or hope their abilities will be in the future.
Have you considered?
- What will happen if one or both of you lose your jobs; divorce; become ill or disabled; reach retirement age and are still in debt without something set aside for the rest of your life and for your loved ones who survive you?
- Do you know which of the five Social Security benefits your child will be eligible to receive at various times in his or her life?
- Have you taken the necessary steps to be assured that your child will remain eligible to receive these benefits?
- Do you know how to leave assets for your loved one’s lifetime care without Medicaid taking some, or all of it as a benefits “payback” before your child receives it?
- Do you want to select the future Guardians and Trustees for your child, or do you want to leave that decision to the State in which you reside?
- If you are divorced, would you like to have someone other than your ex-spouse manage and have control of any assets you leave for your child?
- What happens to the authority you have on behalf of your minor child with special needs when your loved one reaches the age of 18, and becomes an emancipated adult?
These are only a few of the many questions that I hear everyday from parents just like you. Yes, this is a very scary subject and frankly, future planning for your loved one with special needs can be overwhelming. But let’s face reality. Chances are your child with special needs will probably survive you. If you have done no planning, what will happen to your loved one when you die? Who will take care of him or her? Will there be enough money? Scared? Concerned? You should be. I have heard every excuse. No one is more important than planning for the future of your loved one with a disability. Don’t disappoint them by not making sure they will have a safe and secure future when you are no longer here.
Right now, you are probably asking yourself, where can I get the answers to my questions and concerns? Who do I turn to? How do I even begin the planning process? What is it going to cost? How much time will it take? These are all valid questions, not valid excuses. I have answers to all of your questions. But you have to take the first step. You must make the commitment to plan for the future of your loved one. And, it has to be done today, not six-months or 6-years from now, because no one has a crystal ball to see into the future. Not taking action today is just another excuse. Read Part 2 tomorrow, but begin your commitment now by visiting Serenitas Special Needs Planning website at www.SerenitasSNP.com, or call 818-231-6759
If I NeedHelp makes wearable iD and offers a free Caregiver controlled special needs registry for our loved ones who may wander or need assistance in a critical moment.
10 Halloween Driving Safety Tips
BY CARPARTS.COM (reposted with permission)
It’s almost Halloween–that time of the year when kids in costume flock the streets for candy and a night of spooky fun. Despite its festive vibe, statistics show that Halloween is also one of the deadliest nights of the year, when road accidents spike up and according to a study conducted by the University of British Columbia, the risk of pedestrian death increases by 43%. In fact, the fatality rate for children between four and eight years old is 10 times higher on Halloween than on any other day, and the Department of Transportation reported that pedestrian deaths peaked at 5,987 in 2016.
Let these sobering statistics serve as a reminder to us all to take extra precaution and practice defensive driving this season.
What exactly is defensive driving? It’s a set of road skills that, if observed properly, prepares drivers and their passengers for any possible cause of an accident on the road, including bad or drunk drivers, extreme weather conditions, and a lack of familiarity with the area. It’s especially important for avoiding vehicle-pedestrian collisions.
Before you drive out on Halloween night, make sure you review these 10 defensive driving tips:
1. Be extremely cautious when backing into and out of your driveway.
Children judge situations differently than adults, and may not recognize vehicle warning lights. Many could assume that drivers are always aware of them and that they have the go-signal to continue walking. So before you back out of your driveway, take extra precaution and step out of your vehicle to be absolutely sure the coast is clear. When you get back in your car, don’t rely on your back-up camera or rear and side view mirrors alone to see. Make sure to turn your head and look over your shoulder. Rolling your windows down to better hear what’s going on outside also works to support your limited vision while backing up.
2. Drive slower than the speed limit.
The typical speed limit on urban and residential streets ranges from 15 to 40 mph. It is advisable that you drive below these speeds on Halloween because it’ll be especially darker, as some houses will only have jack-o’-lanterns lit and some will have their porch lights off altogether. Compared to a normal night, there’ll also be triple the number of pedestrians on the street, especially kids, so be sure to drive slowly. The slower you go, the shorter distance you need to bring your car to a full stop.

3. Beware of corners and crosswalks.
Apart from driving slower than the speed limit, you also need to be extra cautious when taking corners and passing through crosswalks. Remember to yield before you turn or pass a crosswalk, even when there’s no pedestrian in sight. Children wearing dark costumes can appear out of nowhere, so take more time than usual before you step on the accelerator.
4. Keep an eye out for children.
Keep in mind that kids can behave unpredictably with little idea of the consequences of their actions. Some may even be trick-or-treating unsupervised and run into the street without checking for oncoming vehicles.
Since many children are short, this could present a problem for drivers with relatively bigger vehicles like trucks and a limited field of vision. It is your responsibility as a driver to scan the area and be aware of kids. They could emerge from in between parked cars and be hard to spot if you’re not paying complete attention to the road in front of you. Having properly functioning headlights is especially important since dark streets make children difficult to see. If you’re experiencing problems with your headlights, be sure to replace them immediately before leaving your driveway on Halloween.

5. If possible, drive around the neighborhood with your windows down.
Sometimes while defensive driving it isn’t just about what you can see, but also what you can hear. Since you’re driving in a dark area with kids running around, you may also need to rely on your sense of hearing.
6. Don’t get distracted.
When it comes to Halloween, some houses put on full productions, so we know it’s all too easy to get distracted. However, we urge you to keep your eyes on the road. In that split second you take to look at the decorations, a child could dart across the street.
Also, it’s important that you avoid glancing at your phone, smartwatch, or even your infotainment system’s display as much as possible while driving. A lot can happen in a fraction of a second, so don’t risk it. If you need to use your phone, safely park your vehicle on the side of the road and turn your park lights on.

7. Use your lights and indicators to communicate with other drivers.
Utilize your turn signals, hazard lights, and headlights to communicate with other drivers on the road. Hazard lights will signal cars behind you to approach or pass with caution. Remember to use your turn signals when changing lanes or turning.
8. Report any drunk or reckless driver.
If you happen to see a drunk or reckless driver, immediately dial 911 and report them. Do not follow them or confront them yourself. Either can result in an even more dangerous outcome. Take note of the car’s license plate number and vehicle description (color, make, and model) so you can tell the authorities which vehicle to look for.
9. Do not drink and drive.
If you’re coming from a party where alcohol is involved, make sure there is a designated driver to bring you and your friends home. When faced with a friend who is trying to drive under the influence, stand your ground and insist that they get a ride from someone who is completely sober.
10. Make sure your car is working properly before defensive driving on Halloween night.
Finally, remember to check your brakes, replace failing headlights, and make sure your warning lights are working properly. Driving with any faulty parts will only increase your risk of getting involved in an accident and putting pedestrians at risk.
Stay safe, and have a happy Halloween!
If I NeedHelp makes wearable iD and offers a free Caregiver controlled special needs registry for our loved ones who may wander or need assistance in a critical moment.
Sensory Activities for Autistic Children
A Practical Guide to Home and Classroom Sensory Activities for Autistic Children
by LISA BELLUCK
Reposted with Permission from findreviews.com

Children are naturally playful and love exploring their senses
learning new things about the world around them through sight, touch, taste, smell, and sound. Whether a child is shaking a rattle or putting objects in their mouth, this is known as sensory play. It is an important development for children, especially those who have been diagnosed with autism spectrum disorder (ASD).

Children begin developing at an incredible rate between two and three years old, constantly
exploring and learning new things. Their senses play the most important factor into this. A toddler who touches a pot of boiling hot water, for example, will in the future associate “hot” with pain – but in the future, they may also recognize a pot of boiling water by the steam, and automatically know not to touch it.
Sensory experience is a vital part of brain development and the nervous system, so creating opportunities for children to engage their senses is paramount to their learning. Sensory activities thus stimulate the child’s core senses, building their awareness using textures, sounds, smells, etc.
For example, a child who plays with cups of water, whether they’re splashing the water around or transferring it between containers, is not only developing their sense of touch but learning about the movement of fluids.
With autism, some children are either hypersensitive or under-responsive to their senses, which falls under sensory processing disorder (SPD). This is when the brain finds it challenging to process and respond to the information being sent to it, so an overly-sensitive child may find certain sensory stimulation to be overwhelming.
A lightbulb can be too bright for them, or the simple act of brushing their hair can be painful because their brain sends mixed reactions to the sensory stimulations.Research has stated that over 75% of people with autism also have some type of sensory processing disorder. So for example, if an autistic child is overly sensitive to sounds, they may need to wear headphones to filter out a noisy environment.
Play Therapy UK
an international organization that specializes in sensory play for children, has released numerous findings based on their research:
- Between 74% and 83% of children receiving play therapy, delivered to PTUK/PTI standards, show a positive change.
- The more severe the problems the greater the percentage of children showing a positive change. 74% for those with slight/moderate problems, 83% for those with severe problems.
- Age also has an effect on improvement: Generally speaking the younger the child the greater the percentage of children showing a positive change: 80% at age 6 – 71% at age 12 – early help is the most effective.
- Girls show a higher improvement rate than boys, 79% compared to 73%.
Founding member of Play Therapy UK, Jeff Thomas, explained how PTUK utilizes sensory play with children diagnosed with ASD/SPD:
“Children choose what they want to do in the sessions from a wide range of creative arts therapeutic media. Sensory play forms a large part of session time (60%) through the use of clay, sand trays, water, messy play, drawing and painting, music and puppets – all of which have a sensory element. The Play Therapist communicates with the children using the same medium that the child has chosen, sharing the sensory aspects.”
Another organization, Sensory Trust, also provides sensory play to children with sensory processing disorders. An activity they use often for its multisensory approach, which yields the most benefits, is a simple game called “gofindit”, which is a nature-based scavenger card game.
The scavenger hunt game consists of 33 uniquely designed cards in a small drawstring bag which represent different sensations and sensory characteristics you can find outdoors in nature.
While therapy is highly beneficial to children diagnosed with ASD, there are many simple sensory-based activities you can do at home. We will outline some of the most popular.
Sensory Activities at Home

Coin rubbing
Take a few different coins, and cover them with a sheet of paper. Then have your child to rub over the top of the coin using crayons, which will create images of the coin’s surface. This activity can help to develop an ASD child’s hand-eye coordination skills.

Edible jewelry threading
Your ASD child will love creating their own colorful jewelry, especially if they can eat it afterwards. Candy bracelets can typically be found in supermarkets, so if you buy a bunch of those, then cut the strings and place all the candy in a jar, your child will have their own supply of candy beads to work with.

Put together a sensory activity collage
Because children with ASD can be overwhelmed by new textures and sensations, it helps to ease them into these things with a small collage. Glue items of various textures to a piece of cardboard, such as strips of carpet, pieces of cotton, aluminum foil, felt shapes, and other similar things. You can explain each object to your child, and introduce them to a wider range of textures without overwhelming them.

Ice cube painting
Acrylic paints can be poured into an ice tray, then frozen with wooden craft sticks. When the paints are frozen blocks, allow them to slightly thaw, then let your child swirl the melting paint blocks over a piece of paper. Your child will have fun creating beautiful designs, and it’s certainly less messy than working with liquid paints.

Sensory bottles
A fun project that can yield beautiful results, all you need is a few plastic bottles, a little food coloring, and some things like marbles or colorful plastic shapes. Fill the bottles with water, add a few drops of food coloring, and pour in the rest of the items, finally sealing the lid.
Oobleck
A fun substance that is neither a liquid nor a solid, oobleck is a non-Newtonian fluid that feels solid when pressed together, and oozes like a liquid when released. This is a fun activity and science lesson, and the oobleck properties should be quite amazing to a child with ASD. It is simply a mixture of 2 cups cornstarch, 1 cup of water, and optional food coloring. You can fine-tune the consistency with more food starch or water.

Memory by smell game
Fill a few small containers with fragrant ingredients, then ask your child to identify each smell. Studies show that children with ASD have an acute sensitivity to smell, so be careful not to use any overwhelming fragrances. Some good candidates are coffee beans, vanilla extract, sachets of lavender, etc.
Sensory Aids in the Classroom
It is important to work with your child’s teacher and school staff in creating a plan that benefits your child academically. In the U.S., your child may be given an IEP (individualized education plan), while in the U.K. it is known as SEN (special education needs). These programs are tailored to your child’s disorder, learning ability, and individual needs.
However, communication between parents and teachers is always important, for maximum benefit. There are several sensory play activities that can be applicable to the classroom, and it is worth mentioning these to your child’s teacher.
Classroom bean bag chairs: A simple bean bag chair can contribute to vestibular sensory needs (sense of balance), which is important for ASD children who are commonly prone to rocking themselves back and forth. A beanbag chair will help enable this activity better than a traditional school chair.

Sensory walls and panels: These can help children who require more visual input in class, and can be hung on the wall for children to run their hands over.
Conclusion
Sensory activities are highly beneficial to children with autism (and affiliated SPD), so there are just a few more things to remember.
- Consistency is Key: Children diagnosed with ASD may have difficulty in applying the things they’ve learned in one scenario to others. For example, an ASD child may learn a set of communication techniques at school but does not transition those communication techniques to the home. Consistency is key here, which involves communicating with the child’s teacher and that the child can more easily transfer positive habits between environments.
- Have a structured schedule: Children with ASD perform best under a highly-structured routine, as they can become easily confused, disoriented, and lash out when the world doesn’t make sense to them. The routine should include regular meal times, school, therapy, bedtime, and any other regular daily activities. Any disruptions to the routine should be kept to a minimal. If a routine disruption is unavoidable, it’s important to prepare the child well in advance.
- Use positive reinforcement: Children with ASD react positively to praise, especially in the long-term. It’s important to reward good behavior and be very specific about what exactly they’ve done correctly and earned praise for. This is highly useful when teaching an ASD child a new skill.
- Be aware of the child’s hypersensitivities, if any: Many children with ASD can be hypersensitive to specific senses, so it’s important to be aware of which sensory stimulations can trigger overwhelming stimulation, and avoid them.
If I NeedHelp makes wearable iD and offers a free Caregiver controlled special needs registry for our loved ones who may wander or need assistance in a critical moment.
Is it time to think about Assisted Living?

The decision to help an aging adult move out of a current home is a complex one — both emotionally and practically. Above all, you want the person to be safe and well. How can you all feel more confident about whether circumstances suggest that your loved one should no longer be living alone?
Although every situation is different, looking at the following 11 signs will give you valuable information to help make the decision.
1. Big-picture signs it might be time for assisted living
Keep the big red flags in mind. Certain situations make it more obvious that it’s wise to start thinking about alternate living arrangements.
Look for:
Recent accidents or close calls
Did your loved one take a fall, have a medical scare, or get in a fender bender (or worse)? Who responded and how long did it take? Accidents do happen, but as people get older, the odds rise of them happening again.A slow recovery
How did the person you’re caring for weather the most recent illness (for example, a flu or bad cold)? Was he or she able and willing to seek medical care when needed, or did last winter’s cold develop into untreated bronchitis?A chronic health condition that’s worsening
Progressive problems such as COPD, dementia, and congestive heart failure can decline gradually or precipitously, but either way, their presence means your loved one will increasingly need help.Increasing difficulty managing the activities of daily living (ADLs) and instrumental activities of daily living (IADLs)
ADLs and IADLs are the skills needed to live independently — dressing, shopping, cooking, doing laundry, managing medications, and so on. Doctors, social workers, and other geriatric experts evaluate them as part of a functional assessment, which is one way to get an expert’s view of the situation. Difficulties with ADLs and IADLs can sometimes be remedied by bringing in more in-home help.

2. Up-close signs it might be time for assisted living
Give your loved one a big hug. Clues aren’t always visible from a distance; especially when you don’t see the person every day, you might learn more through touch.
Look for:
Noticeable weight loss
Does the person feel thinner? Are clothes loose, or has he added notches to his belt? Many conditions, from depression to cancer, can cause weight loss. A person who is having trouble getting out to shop or remembering how to cook (or to eat) can lose weight; check the fridge and watch meal-prep skills.
Seeming more frail
Do you feel anything “different” about the person’s strength and stature when you hug? Can your loved one rise easily from a chair? Does she or he seem unsteady or unable to balance? Compare these observations to the last time you were together.Noticeable weight gain
Common causes include an injury slowing the person down, diabetes, and dementia (when someone doesn’t remember eating, he or she may indulge in meals and snacks all day long). Someone with money troubles may choose fewer fresh foods and more packaged goods or dried pasta and bread.Strange body odor
Unfortunately, a close hug can also reveal changes in personal hygiene habits. Causes range from memory trouble to depression to other physical ailments.Changes in appearance
Does the person’s hair and makeup look all right? Are clothes clean? Someone known for crisply ironed shirts who’s now in a stained sweatshirt may lack the dexterity for buttons or may have lost the strength for managing an ironing board and iron. A formerly clean-shaven man with an unkempt beard may be forgetting to shave (or forgetting how to shave).
3. Social signs it might be time for assisted living
Think realistically about the person’s social connections. Social circles tend to shrink with age, which can have health and safety implications.
Look for:
Signs of active friendships
Does your loved one still get together for lunches or outings with friends or visits with neighbors, or participate in religious activities or other group events? Does he or she talk about others or keep a calendar of appointments? Lack of companionship is associated with depression and heart problems in older adults. If friends have died or moved away, moving to a place where other people are around could be lifesaving.Signs that your loved one has cut back on activities and interests
Is a hobby area abandoned? Has a club membership been given up? A library card gone unused? There are many reasons people cut back, but dropping out of everything and showing interest in almost nothing is a red flag for depression.Days spent without leaving the house
This sometimes happens because the person can no longer drive or is afraid to take public transportation alone and lacks a companion to come along. While many older adults fear being “locked away” in a retirement home, many such facilities offer regular outings that may keep them more mobile and active, not less.Someone who checks in on a regular basis
If not you or another family member, who does this? Is your loved one willing to consider a home-safety alarm system or medical alert system?
A plan for a worst-case scenario. If there’s a fire, earthquake, flood, or other disaster, is someone on standby to assist? Does your loved one understand the plan?

4. Financial signs it might be time for assisted living
Rifle through the mail. Your loved one’s mail can offer an often-overlooked clue to how he or she is managing money, a common early warning sign of cognitive trouble.
Look for:
Snowdrifts of mail in various places
Finding lots of mail scattered around raises concern about how bills, insurance, and other matters are being managed. (Piles of mail are also a potential tripping hazard.)Unopened personal mail
Everybody skips junk mail, but few of us can ignore a good old-fashioned, hand-addressed letter.Unopened bills
This can indicate that your loved one is having difficulty managing finances — one of the most common first signs of dementia.Letters from banks, creditors, or insurers
Routine business letters aren’t worrisome. But it’s alarming if they’re referring to overdue payments, overdrawn balances, recent accidents, or other concerning events.Thank-you messages from charities
Older adults are often vulnerable to scammers. Even those who have always been fiscally prudent are vulnerable if they’re having trouble with thinking skills (a common sign of Alzheimer’s disease). Some charities hit up givers over and over, and your loved one may not remember having donating the first time.Lots of crisp, unread magazines
The person may unknowingly have repeat-renewal subscriptions that he or she doesn’t need.
5. Driving signs it might be time for assisted living
Take a drive — with your loved one behind the wheel, if he or she is still driving. Often, the ability to drive is practically a requirement for living independently in our culture (or the arrangement of alternate transportation options).
Look for:
Nicks or dents on the car
Notice the car body as you get in and out. Damage marks can be signs of careless driving.Whether the person promptly fastens his or her seatbelt
Even people with mild dementia usually follow the rote basics of driving. It’s worrisome if he or she is forgetting this step.Tension, preoccupation or being easily distracted
The person may turn off the radio, for example, or be unwilling to engage in conversation while driving. He or she may avoid certain routes, highway driving, or driving at night and in rain — a safe kind of self-policing but also signals of changing ability.Signs of dangerous driving
People whose driving ability is impaired are more likely to tailgate, drift from their lane, go below the speed limit, react slowly to lights or other cars, and mix up gas and brake pedals. See 8 ways to assess someone’s driving.Warning lights
Check out the dashboard as you ride along. Does the car have sufficient oil, gas, antifreeze, windshield-wiper fluid?

6. Kitchen signs it might be signs for assisted living
Go through the kitchen, from fridge to cupboards to oven. Because people spend so much time in this room, you can learn a lot.
Look for:
Stale or expired foods
We all buy more than we need. Look for signs that food is not only old but that this is unnoticed — mold, sour milk that’s still used, or expiration dates well past due, for example.Multiples of the same item
Ten bottles of ketchup? More cereal than can be eaten in a year? Multiples often reveal that the shopper can’t remember from one store trip to the next what’s in stock at home.A freezer full of TV dinners
Your loved one may buy them for convenience sake, but frozen dinners tend not to make healthy diet. If there’s not much fresh food in the house (because it’s too hard to for the person to procure or cook), your loved one might be ready to have help with meal prep or delivery services.Broken appliances
Check them all: microwave, coffeemaker, toaster, washer, and dryer — any device you know your loved one uses (or used to use) routinely.Signs of fire
Are stove knobs charred? Pot bottoms singed badly (or thrown out)? Do any potholders have burned edges? Also look for a discharged fire extinguisher, smoke detectors that have been disassembled, or boxes of baking soda near the stove. Accidents happen; ask for the story behind what you see. Accidental fires are a common home danger for older adults.Increased use of takeout or simpler cooking
A change in physical or mental abilities might explain a downshift to simpler recipes or food choices.

7. Around-the-house signs it might be time for assisted living
Look around the living areas. Sometimes the most obvious sign is hard to see because we become so used to it.
Look for:
Lots of clutter
An inability to throw anything away may be a sign of a neurological or physical issue. Obviously it’s more worrisome in a neatnik than in a chronic slob. Papers or pet toys all over the floor represent a tripping hazard.Signs of lax housekeeping
Spills that haven’t been cleaned up are a common sign of dementia — the person lacks the follow-through to tidy. Keep an eye out for cobwebs, bathroom mold, thick dust, or other signs of slackness. Physical limitations can mean your loved one needs housekeeping help or a living situation where this is taken care of for him or her.Bathroom grime and clutter
A common scenario: Your loved one makes an effort to tidy up living areas but overlooks the bathroom. Or the guest bath is clean, but not the one the person uses all the time (the one off a bedroom, for example). Here you may see a truer picture of how your loved one is keeping up.
8. Pet-care and plant-care signs it might be time for assisted living
Be sure to check out how the other living things are faring. An ability to take care of pets and plants goes along with self-care.
Look for:
Plants that are dying, dead or just gone
Most of us have seen plants go brown sometimes. Keep an eye out for chronic neglect, especially in a former plant-lover’s home.Animals that don’t seem well tended
Common problems: dogs with long nails, cat litter boxes that haven’t been changed lately, or dead fish in the fish tank. Poor grooming, overfeeding, and underfeeding are other red flags.
9. Home Maintenance signs it might be time for assisted living
Walk around the yard. Yard maintenance — or lack of it — can yield clues that your loved one isn’t faring as well at home alone anymore.
Look for:
Signs of neglect
Look for discolored siding or ceilings that might indicate a leak, gutters choked with leaves, broken windows or fences, dirty windows.Newspapers in the bushes
Are papers being delivered but ignored? Sometimes people pick up those they can see on a driveway but not those that go off into the yard.Mail piled up in the mailbox
Go out and check — it’s an indication that your loved one doesn’t even retrieve it regularly.

10. Get help looking for signs it might be time for assisted living
Get the input of others who know your loved one in order to collect a fuller picture of reality.Gently probing about what others think isn’t nosy; you’re being loving, concerned, and proactive.
Look for:
Input from those in your loved one’s circle
Talk to old friends and close relatives to get their sense of how the person is faring. Listen for stories that hint that the person doesn’t get out much (“She doesn’t come over anymore.” “She quit book club.”). Pay attention to comments that indicate ongoing concerns (“Has he had that heart test yet?” “We were worried the day the ambulance came.”).Medical insight
With appropriate permission, your loved one’s primary doctor may share your concerns about his or her patient’s safety at home — or may be able to alleviate those concerns or suggest where to get a home assessment.A second opinion
A social worker or professional geriatric care manager visits older adults’ homes and does informal evaluations. While your loved one may initially resist the notion of a “total stranger” checking on them, try pitching it as a professional (and neutral) second opinion, or ask the doctor to “prescribe” it. Some people wind up sharing doubts or vulnerabilities with a sympathetic, experienced stranger that they’re loathe to admit to their own children or family.
11. Caregivers’ signs it might be time for assisted living
Finally, realize that some of the information you collect is intangible — it has to do with feelings and emotions, and the stress levels of everyone involved.
Look for:
How you’re doing
While this decision to remain in one’s home is not primarily about you — the son, daughter, grandchild, caregiver — your own exhaustion can be a good gauge of a decline in older adults’ ability to care for themselves. Keeping someone at home can require lots of hands-on support or care coordination, and this is time-consuming. If your loved one’s need for care is just plain wearing you out, or if a spouse or children are feeling the collective strain of your caregiving activities, these are major signs that it’s time to start looking at other options.Your loved one’s emotional state
Safety is crucial, of course, but so is emotional well-being. If someone living alone is riddled with anxieties or increasingly lonely, then that may tip the scales toward a move not solely based on health and safety reasons.
If your loved one has a full life, a close neighborhood and community connections, and seems to be thriving, it’s worth exploring as many in-home care options as possible before raising stress levels by pressing a move from a beloved home.If, on the other hand, your loved one is showing signs that living alone is a strain, it may be time for a talk. Broach the subject of where to live in a neutral way and you may find that your loved one harbors the same fears for current and future safety and security that you do. Find out what your loved one fears most about moving and about staying before launching into your own worries and what you think ought to be done.
If I NeedHelp makes wearable iD and offers a free Caregiver controlled special needs registry for our loved ones who may wander or need assistance in a critical moment.
Medical Alert Devices for the Elderly
Written by consumersadvocate.org

How To Find the Best Medical Alert Device
If you have an older parent, husband or friend that is not able to take care of themselves on their own, it’s not only disheartening, but can be hard on everyone. It’s hard enough that you need to be the one addressing all their needs, emotionally and physically, but then there is also the added task of convincing your loved one that they need to let you be in charge.
If you are in that position or even have hired a caregiver to help care for your loved one, a medical alert system can be a big help and relief for everyone. Medical alert devices can help a caregiver or whomever is looking after the senior in question to call for help if necessary.
Medical alert devices are not only imperative, but can even save a person’s life. If the senior in question is wearing a device and still has the ability to think on his or her own, he can get in touch with you, a caregiver or even emergency services if they have fallen or have been hurt.

How Medical Alert Devices Work
If your loved one or even a caregiver presses a medical alert button, they will be connected automatically to a monitoring service where the trained specialist that answers the phone can assess the situation and call the appropriate hospital or emergency services.
Some companies will also have the medical information of the senior in question in their records to help gauge the situation.
There are many different medical alert devices that will have the ability to protect your father or mother who is not only at home but if he wanders. Some of these devices have motion sensors that can help if your loved one falls or is any area of the home that poses more of a threat to themselves such as the top of a staircase.
Some questions to consider to help you choose the best medical alert device:
- Is the senior able to press a medical alert button in an emergency?
- Is it best to choose a device that is more specific for a person that wanders?
- Would you elderly loved one press the button too many times by accident?
What Types of Medical Alerts are Available?

When medical alert devices first became available, they were usually in the shape of a pin-style button that connects to a base station and hooked to a home phone landline. This was helpful but only for those who rarely left home.
Today, since technology has improved greatly, there are many different combinations of base stations and pendants that can be tracked much further. And, of course, this can be a very important feature for those that wander.
There are even mobile-phone based services that use a cell phone instead of a landline to connect. This feature can be great for those with dementia because they have a GPS position function to allow caregivers to know the exact location of the senior.
There are also different devices that contact the responsible caregiver if the senior falls or hurts themselves and can’t get to a phone on his own for help. As most of us know, falling is very common among the elderly.
Now that you have decided to purchase a medical alert system, there are some other things to consider before purchasing one.
The Equipment of the Device
It’s important to learn how the different systems work, the different components they include and how to maintain them.
With older systems, home bases will not work if the alert button isn’t close by.
If the senior has limited mobility, then you need to make sure to purchase a unit that has an alert button close to the base unit in every room that he or she might enter.
Contract
Of course, as with anything you purchase, it’s important to read the contract thoroughly to understand how the service works, how long the agreement is, trial periods and cancellation.
Many providers will offer discounts for longer-term contracts or if you pay more up front for the entire year.
Compare Pricing
Once you learn the best system for your needs, it’s important to get a few quotes to compare pricing.
Try to find the company that has the best system and service for the best price.
Read Customer Reviews

Once you’ve narrowed down the device you want and the price, the next thing to consider is how customers like the service.
Some things to consider:
- Does the service offer a trial period so you can test out the system?
- Is there any easy return policy or cancellation of the service if you aren’t satisfied?
- And, most important, does the system work well in the event of an emergency?
If you can find positive answers to all of the above, you can feel assured that you should have a good experience with the company and specific medical alert device.
Medical alert devices for your loved one are one of the most important devices that you will buy. With a little research, you will find the best medical alert device that will give you the reassurance that your elderly loved one or caregiver always has a way to get in touch with you or medical help if necessary.
consumersadvocate.org has created an in-depth review of some of the top Medical alert devices to help you make your choice.
If I NeedHelp makes wearable iD and offers a free Caregiver controlled special needs registry for our loved ones who may wander or need assistance in a critical moment.
Keeping Your Child with Autism Safe
Reposted with permission from safety.com

A recent study by the American Journal of Public Health examined national mortality data and found that individuals with a diagnosis of autism died on average 35.8 years younger than individuals in the general population. Their research also found that the difference in deaths caused by injury was almost as striking.
Most parents place their children’s safety as a top priority as a rule. But for parents of children with autism, the reality is that it can be even more difficult to keep your children safe from themselves and others simply because of the nature of their disorder. However, parents of children with autism should not live in constant fear: there are tips parents and caregivers of kids with autism can follow to make sure they stay safe.
Characteristics of Autism
People with ASDs (autism spectrum disorders) share some symptoms, such as difficulty with social interaction, and their brains process information differently than those of unaffected people. Children with ASDs may exhibit a common set of characteristics that naturally make them more susceptible to danger. For instance, people with ASDs commonly have no real fear of dangers and an apparent insensitivity to pain. An inappropriate response—or no response at all—to sound is another common characteristic that could open the door to danger.
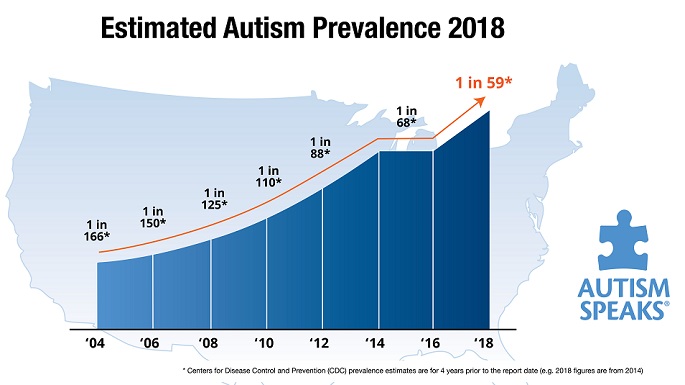
Estimated Autism Prevalence 2018
Scientists do not yet know the cause of ASDs. According to the CDC, ASDs occur in people of all racial, ethnic, and socioeconomic backgrounds. While it is estimated that autism affects 1 in 88 children, boys are nearly five times more likely than girls to be affected by autism; in fact, the number of boys affected by autism is 1 in 54, compared to 1 in 252 girls. And, Autism Speaks points out that the prevalence of autism is not just growing: it is “the fastest-growing serious developmental disability in the United States.”
Keeping all children safe is important. But, keeping children with autism safe becomes even more of a priority because of their social, communication, and behavioral challenges.
5 Tips for Creating a Safety Plan
Autism Speaks recommends that parents of children with autism create safety plans, and there are some basic tips to keep in mind when creating those plans for your child with autism.
1) Include family and community members who come into daily contact with your child with autism. Keep in mind school personnel, daycare providers, neighbors, extended family, etc. Make sure you have contacted each person and discussed your most pressing concerns about your child’s safety.
2) Think about all of the places in which your child needs to be protected. This probably includes home, school, friends’ homes, community centers, etc. Then, be sure to evaluate them for safety and to put preventative measures into place in each area. It is especially important to remember to include safety skills in your child’s Individual Education Program (IEP) in your school district.
3) Consider the top safety risks for individuals with autism: wandering, pica (the tendency to eat or crave substances other than normal food), drowning, and household toxins. Take the necessary precautions for safeguarding your child against these safety risks and practice safety skills with your child other family members.
4) Give your child a form of identification with contact names and numbers listed. Make sure your child always wears or carries this identification, especially because wandering could be a concern. Or, purchase a child locator and clip it to your child’s shoe, belt, etc. (All these products and more are available at IfINeedHelp.org)*
5) Contact your local communications center, police department, and/or 911 call center to communicate your concerns and safety plan with the appropriate officials. Remember, you are your child’s best safety advocate.
Safety at Home
The home can be a very dangerous place for any young child, but it can be even more dangerous for your child with autism. The difference is that the safety measures and precautions most parents implement for very young children may need to be in place for a much longer period of time for children with autism. Consider this checklist to keep your child with autism safe at home
- Furniture – Secure especially top-heavy furniture to the wall with furniture brackets or safety straps. Don’t forget that some electronics also may be heavy or easily pulled over by your child, so use items such as TV safety straps.
- Cleaning products – All cleaning products should be locked in a safe location. You may want to put them in a locked area in the garage or basement, so they are not in the main living space of your home.
- Freezers – If you own a chest-style freezer, keep it locked at all times. Storing the key in a safe place where your child cannot access it is a good idea.
- Doors – Key locks may be enough for some children affected by autism, but you may want to use door alarms to prevent your child from leaving your home without your knowledge. Again, remember to keep your keys in a place out of your child’s reach. If your child has been known to wander (see the section on wandering below), you should use a child locator. There are several types available, especially online, but any you choose would help ease your mind about your wandering child.
- Visitors – As with any child, you should teach your child with autism the safety rules about opening the door to visitors, especially if he is home alone. The old safety rule of not opening the door to anyone when home alone is especially important for an child with autism who has a severe language or speech delay or who is completely nonverbal. One way to communicate this rule to your child with autism is to create a social storybook with pictures to help explain the rules.
- Hot water – Sometimes children with autism struggle with sensory challenges, so they may be more at risk for getting burned by hot water simply because they cannot feel hot and cold. One simple solution is to turn down the temperature on your hot water heater. If you have an older child with autism, you may want to practice turning on the hot water with the cold water. You may even put stickers on the hot water knob to remind your child that it is a potential danger to him. Don’t forget to do this in the shower as well as on your sink faucets.
- Fire – As with all children, practicing for a house fire is an important safety measure. Some children with autism may become frightened of the loud alarms in your home, so you may want to purchase a smoke detector that records your voice rather than a traditional one. Another fire safety tip is to take your child to your local fire department so he can become familiar with the firemen and the gear they wear when they enter your home because some children with autism handle stressful situations better when they have experience with them beforehand, in a calmer setting.
- Swimming Pools – If you own a pool, fence it in and make sure your gates are self-closing and latch above your child’s reach. Keep all pool toys and other interesting items out of the pool area when they are not being used. Ask your neighbors with swimming pools to follow these safety tips and make them aware of your child’s potential for wandering. Prior to the Danish study on mortality rates in people affected by ASDs, a California research team pointed to drowning as the cause of the elevated death rate of individuals diagnosed with an ASD, so swimming pool and water safety lessons are crucial for children with autism.
Kids with Autism Wandering Away from Home
A recent study funded by Autism Speaks, through its support of the Interactive Autism Network(IAN), an online project bringing together families affected by autism, and published in the journal Pediatrics shows that children with ASDs wander away from home, stores, and school more often than unaffected children. Through the use of parent surveys, researchers found that nearly half of children with autism attempt to wander or run from a safe, supervised place, and more than half of these wandering children go missing long enough to cause worry. Of the children who caused worry, 65% of the incidents involved a close call with traffic, and 32% involved near drowning.
Overall, the occurrences of wandering increased with the severity of the ASD, and the children who wandered most commonly left their own homes or ones they were visiting. Most parents listed the main reason for their child’s wandering as being their enjoyment of running and exploring, but other reasons included visiting a favorite place or escaping a stressful situation or an uncomfortable sensory stimuli. The study highlighted the need for parents to develop safety plans with their families, teachers, police, and other community members to protect children with autism who wander and to be able to locate them.
6 Tips to Help Prevent Wandering

The National Autism Association recommends that parents and caregivers use the following tips to help prevent wandering by understanding wandering patterns and eliminating triggers in children with an ASD:
1) Determine which type of wandering best describes your child (is he directed by goals, is he a sudden runner, etc.).
2) Recognize what triggers the wandering incidents.
~If it is a goal, allow the child to explore the goal in a safe and supervised manner (for example, if the child’s goal is to get used to water, schedule a time for water play each day).
~If it is to escape something, address the issue (for example, there may be too much noise at a certain time of day that the child is trying to get away from).
3) Develop and implement strategies to help your child deal with his triggers in a way that helps him to cope with the trigger rather than running away.
4) Include known triggers in your child’s IEP so that he may work on calming techniques with the appropriate school personnel.
5) Acquire appropriate social stories and review them with your child.
6) Share your child’s goal, fascination, or need to escape with all people who are involved in your child’s daily routine to aid them in preventing your child from wandering.
Moreover, the Autism Wandering Awareness Alerts Response and Education (AWAARE) Collaboration is working toward reducing autism-related wandering incidents and deaths. Some of the tips they specifically recommend for parents of wandering children with autism include the following:
~ Contact a professional locksmith, security company, or home improvement professional to promote safety and prevention in your home.
~ Get a tracking device for your child with autism such as Angelsense or check with local law enforcement for Project Lifesaver or LoJack SafetyNet services.
~ Have your child wear an ID bracelet or necklace that includes your name, telephone number, and other important information. If your child with autism will not wear a bracelet or necklace, consider a temporary tattoo. (All these products and more are available at IfINeedHelp.org)*
~ Teach your child to swim, but remember that teaching a child to swim does not mean he is safe in or near water.
~ Introduce your neighbors to your child with autism and provide a photograph with your name, address, and phone number so they can call you immediately if they see your child outside of your home. (You can use IfINeedHelp.org neighbor alert with their free membership)*
~ Provide first responders with key information on handouts (you should distribute these to your family, neighbors, friends, and coworkers as well): include the name, age, and physical description of your child with autism as well as his favorite song, toy, or character so the first responders are able to communicate with and calm your child more easily. (You can use IfINeedHelp.org emergency questions and answers with their free membership)*
Safety at School
Because children spend such a large amount of time in school, it is just as important to know how to keep them safe in the classroom as it is at home. The following six tips should help to keep your child with autism safe in their home-away-from-home.

- Visit your child’s school and classroom prior to the start of the school year. Evaluate the building in the same way that you evaluated your home. Are there doors and windows that lock? Can your child reach the locks? Is there any water nearby? Are there any sensory triggers that could result in your child running away? Are there times when your child will be transitioning from one place to another without supervision?
- Take your child to school prior to the start of the school year. Show him his classroom and the restroom facilities and introduce him to faculty and staff.
- Schedule a meeting with all of the faculty and staff who will be in contact with your child. Give them copies of the key information handouts and share your concerns with them.
- Schedule an IEP meeting before school begins and a follow-up meeting once the school year is underway. Be an active participant and advocate for social skills, safety training, and learning goals to be included and evaluated as part of the IEP process.
- Meet with the principal about the school’s policy on bullying. A study published in Archives of Pediatrics & Adolescent Medicine found that about 46% of children with autism in middle and high school reported to their parents they had been victimized at school within the previous year, compared with just over 10% of unaffected children.
- Also, ask the principal about the school’s use of restraint and techniques for calming students with autism. An ABC News investigation found that in recent years, thousands of children have been injured and dozens killed after being restrained at school.
Safety in Public
Because of the unpredictable nature of going on an outing, one of the most important things you can do is prepare your child with autism before going to a public place. Telling your child where you are going and why may ease his anxiety about changing the routine of his day and may prevent a meltdown. Health Central recommends a few things that may make the preparation for the outing easier for your child and yourself.
- Use pictures so the child can become familiar with the new place. This will also give you an opportunity to discuss some safety measures you may take with your child, such as holding hands when you cross the street, watching for the appropriate signal before crossing the street, etc.
- Tell social stories or listen to social narratives (Rock the Fish)* to describe the public place and the relevant skills that will be needed to have an enjoyable outing. Remember to emphasize something that an individual does well, so that your child will have a better understanding of what he should do in the public place you are going to visit.
- Explain what will happen when you go on the outing. There is no way that you can anticipate everything that will occur, but you can highlight key points and reassure your child that he will enjoy himself. And, if something unexpected happens, remain calm so that your child does not pick up on your level of anxiety.
- Create a schedule and plan activities that your child enjoys. You should be prepared to keep your outing short and your expectations reasonable.
- Practice traffic safety rules and role-play public outing scenarios. For example, when you cross a street, verbalize the rules and then have your child recite them as you cross the street. Follow this routine each time you cross a street. This behavioral skills training is critical to a child with autism’s understanding of public safety rules and has even better effects when a parent or teacher trains the child in more realistic situations.
Whether your child with autism is home, at school, or in a public space, make sure you have equipped him with the materials, skills, and knowledge necessary to stay safe. Remember, you are his best safety advocate.
More Safety Solutions for Kids and Families:
- Safest Convertible Care Seats
- Digital Cameras for Kids
- Best Baby Proofing Products
- Smart Home Systems
- Smart Home Security Products
- Home Automation Products
If I NeedHelp makes wearable iD and offers a free Caregiver controlled special needs registry for our loved ones who may wander or need assistance in a critical moment.
* added by If I Need Help
Dental Care for kids with communication issues

5 Signs Your Child May Have Dental Issues and How to Spot Them
By Dr. Greg Grillo
Sometimes, when a child is in pain it is easy for them to communicate that pain to their parent or guardian. However, for children with autism, they may be nonverbal. This means they could be in intense pain or discomfort without anyone knowing. This can make it difficult when it comes to dental issues in your child. Dental issues can arise at any time and can become extremely serious if left untreated. It’s a terrifying fear that exists amongst both children and parents. As a parent, you never want to see your child’s life at risk. I have been practicing family dentistry for 17 years and the safety and comfort of your family is always my number one priority. That’s why I’ve compiled a list of signs that your child may have dental issues and how you can spot them and get treatment as soon as possible.
1. White or Brown Spots
If you notice any chalky white spots on your child’s teeth, it may be a sign that a cavity is developing. Even more so, if the tooth is turning brown or black, you need to visit a dentist as soon as possible. Tooth decay can progress quickly, so any discoloration must be dealt with immediately. Children who are most at risk for cavities and tooth decay are those with high levels of bacteria in their mouth, those with a diet high in sugar and starches, those with poor oral hygiene, and those who have less saliva flow than normal. The best way to check for any discoloration or tooth decay in your child’s teeth is to examine their teeth every once and awhile. A cavity is usually not painful which is why it’s important to check occasionally. Regular examinations, daily brushing and flossing, along with regular dental visits can assure that your child doesn’t get any cavities
2. Irritated Gums
When checking your child’s mouth, another thing to look for is irritated gums. If their gums are irritated they will be red, swollen, and maybe bleeding. This is a sure sign that you should head to the dentist as irritated gums usually indicate gum disease or other health concerns. Like cavities, gum disease can be painless so you’re child may not know anything is wrong. Also similar to tooth decay, gum disease can also spread rather quickly and lead to more serious issues which is why it’s important to see a dentist as soon as possible. This condition is one of the most serious and your child can develop abscessed teeth because of it. The best time to check your child’s mouth is in the morning and night when they practice brushing their teeth.
3. Abscessed Teeth
Abscessed teeth, also known as oral infections, are one of the most serious dental conditions and you should look closely for any oral infections in your child. They can be caused by both tooth decay and gum disease. These can often go unnoticed until it’s too late. A lot of children with autism are nonverbal which can make spotting an abscessed tooth even more difficult. If your child is nonverbal be sure to regularly check their mouth for any signs of an oral infection. Oral infections thrive near the gums and one sure sign of an abscessed tooth are pimple like bumps on the gums. If you notice this in your child, head to the dentist right away. If the infection goes untreated it can become much more serious as it may spread to other parts of the body.
4. Bad Breath
Bad breath can seem like a normal issue that can have an easy fix. Usually, this is the case. However, in some instances, bad breath can be a sign of inflamed gums, dry mouth, or be related to other medical issues your child may have. Some underlying medical issues that may cause bad breath are swollen tonsils and sinus infections. Visiting a dentist regularly and having a good oral care routine at home are good ways to prevent bad breath and most dental issues. However, if you notice that your child has bad breath that won’t go away with regular dental care, head to your dentist or primary healthcare provider to find out if there are any underlying medical issues.
5. Teeth Grinding
Teeth grinding, or Bruxism is a common dental issue amongst children and especially children with autism. Teeth grinding usually doesn’t result in anything serious and can be an easy habit to break with fidget toys and other items. However, some more serious issues that can arise from prolonged teeth grinding are wear on the teeth, jaw pain, and headaches. It’s important to work to break this habit before more serious issues arise, and before your child gets any of their permanent teeth. Prolonged teeth grinding on permanent teeth can cause more wear and damage than on baby teeth.
Special Needs Dental Care issues in children can be serious if left untreated. For children with autism, it can be more difficult to uncover these issues. However, regularly checking your child’s mouth and staying alongside them as they practice dental hygiene is a great way to spot issues before they become more serious. Embrace the journey of learning about dental care together and enjoy learning the best ways to care for your teeth together. If you do notice any issues, call your dentist and schedule an appointment right away. Dental issues can quickly become more serious and you will want your child to receive treatment as soon as possible.

Dr. Greg Grillo was born and raised in the Okanogan Valley in Washington state. Dr. Grillo spent eight years at the University of Washington and received a bachelor’s degree with honors before attending the School of Dentistry on the same campus.
From there he was selected for a Health Professions Scholarship by the United States Navy where he served as a dental officer for four years. After treating families of squadron military members in South Carolina and Japan, Dr. Grillo returned home to join his father’s practice where he has remained for more than 17 years.
Dr. Grillo’s more than two decades of expertise, combined with his passion for dental marketing and knowledge of dental software, makes him an invaluable asset to the Emergency Dentists USA team.
And because he’s still working as a dental practitioner and constantly taking new courses to stay educated, he knows better than anyone what our readers and callers can expect when they visit an emergency dentist, as well as what to look for when we partner with practitioners across the United States.
If I NeedHelp makes wearable iD and offers a free Caregiver controlled special needs registry for our loved ones who may wander or need assistance in a critical moment.





